As we near the end of our second year of pandemic, the world grapples with yet another variant.
On November 20, The New York Times entertained the tantalizing thought of an end to mask mandates, remarking on “the summer’s Delta surge in the rearview mirror.” Unfortunately, the coronavirus didn’t get the memo. Just four days later, on the 24th, South Africa reported a new COVID-19 variant of concern to the WHO — a variant that has since been dubbed omicron and is creeping its way around the world.
The omicron variant poses a number of questions for all of us. How should we react to this variant — as individuals, nations, and globally — to maximize our safety? What can we do to take more effective preventative measures so that more concerning variants don’t keep cropping up? How do we improve global vaccine equity? Furthermore, did you know they skipped two letters of the Greek alphabet to name the new variant? (How ever will we learn the Greek alphabet in order now?)
So Much Remains to Be (Vac)cine
Since the omicron alarm was raised, scientists have raced to determine the implications of its numerous mutations, and nations across the globe have raced to impose travel bans on South Africa. While travelers from African countries face intense travel bans, the variant has been identified in over 50 countries, including much of Europe and the United States. Curiously, travelers from these northern countries have not been subject to the same level of scrutiny.
Predictions about the increase in omicron’s transmissibility warred with nervous optimism that it appeared to be causing less severe illness for the small and relatively young populations in which it’s been observed. Scientists, though, warn that evidence of the variant’s actual severity may come very late and that its higher transmission rate poses great risks regardless of its severity.
The omicron variant may prove a wrecking ball to the dream of herd immunity, according to an interview with a member of the South African research team that notified the WHO about omicron. In initial observations of the new variant in PCR tests, scientists discovered that it was able to evade one of the three probes in the test for the coronavirus. In the same vein of not-so-fun surprises, omicron has been found to excel at reinfection and breakthrough infection, posing a threat to those who have already had prior infections or full vaccination. This finding has kickstarted a host of trials to determine the effectiveness of our existing vaccines on the new variant.
A third dose of the Pfizer vaccine is now recommended to protect against omicron, and booster shots are being hailed all around. The guidelines on what booster shot to take are surprisingly — and nerve-wrackingly — vague. Three vaccines — Pfizer-BioNTech, Moderna, and Johnson & Johnson — now offer booster shots, and vaccine mixology is highly encouraged. Supported by clinical trial data, experts say that the goal is boosting your antibody levels, and that after full vaccination, it doesn’t matter what name the next dose comes under.
Making Haste and Causing Waste
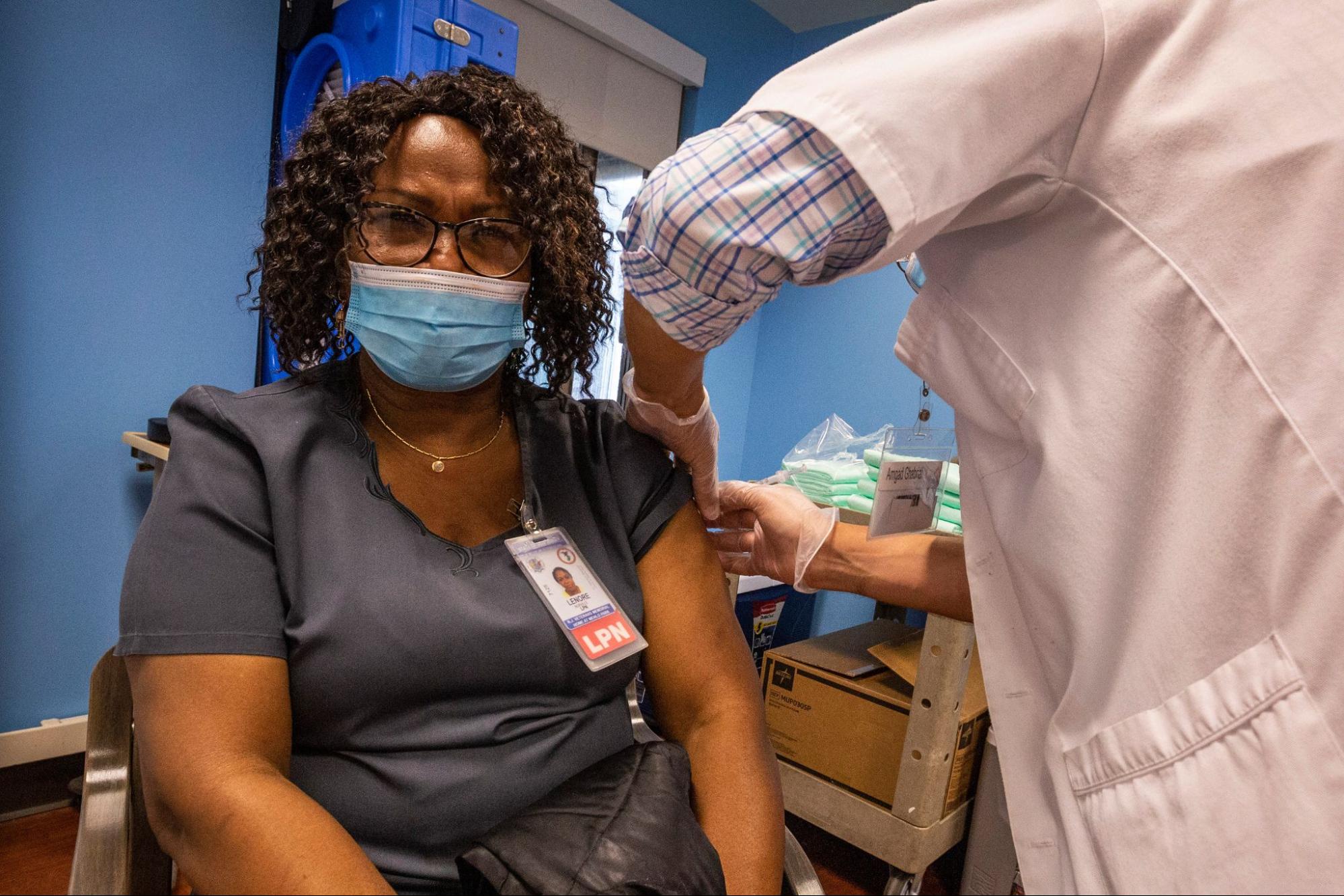
Inequity in vaccine distribution has been a gaping wound of shame for the past year. Although more than 8.43 billion COVID-19 vaccines have been administered around the world, “The least wealthy 52 places have 5.6% of the vaccinations but 20.5% of the world’s population.” The WHO identifies the distribution failure as “not a supply problem; [but] an allocation problem.” The disparity can be rectified if vaccine distribution focuses on at-risk groups and health care workers. It’s the least we can and should do, especially when valuable vaccine doses are taken for granted by the privileged (we could really use a hand getting out of this pandemic, but something tells us silicone isn’t the answer).
All I Want for Christmas Is a Protein Subunit Vaccine
Protein subunit vaccines for COVID-19 were in development in 2020 at Novavax and Sanofi. Both companies ran into issues that prevented their rollout, but now Novavax says it is ready to produce vaccines in 2022. And even though we’re now many vaccines into the pandemic, the protein subunit vaccine still offers immense benefits: It’s easier to store, reportedly easier to manufacture than mRNA vaccines, and less likely to produce severe side effects.
As the holidays head our way, people all over the US are asking familiar questions about travel and celebration guidelines. Given that multiple COVID-19 variants are still circulating, the answers to these questions should probably be familiar by now, too. Yet, like many of the family relationships we’ll be dealing with over the holiday season, somehow, it still manages to be “complicated.”
Vaccination, testing, and travel requirements vary wildly by nation, state, and choice of vehicle. The CDC offers holiday “tips” and “considerations” rather than hardline recommendations. Interestingly, state and federal governments alike have data that finds that mask and vaccine mandates encourage more folks to take preventative measures. Yet, for some, mandates and their seeming oppression of autonomous choice greatly reduce interest in mask-and-vax. With a dearth of definitive answers and an abundance of pandemic fatigue, the right things to do may be obvious; getting ourselves to do them is less straightforward.
And a Happy New Year
If there’s a positive angle to COVID-19, it may be in your New Year’s resolutions. A survey by Fidelity Investments found that over 71 percent of folks kept their 2021 resolutions, a significant jump from the 58 percent who kept them in 2020. The pandemic forced us to slow down and make more mindful decisions about how to spend our money and our time. And in a world of uncertainty, we can regain a sense of control by saving money, doing a home workout three times a week, or even simply making our bed every day.



