As worries grew about claims of menstrual changes caused by the Moderna vaccine, one question remains; why doesn’t science know more about periods and vaccines?
On February 24, Kathryn Clancy took to Twitter to ask her followers if they noticed anything different about their periods. Clancy, an associate professor at the University of Illinois, had received the first dose of the Moderna vaccine a few days earlier and was already experiencing a drastically heavier flow than normal.
The post gained traction as hundreds started commenting on the changes they noticed to their own menstrual cycles, or the experiences they were hearing about from others. Some were concerned, but Clancy was more intrigued than anything else.
“Does this have to do with the way the vax response is mounting a broader inflammatory response, possibly more so because of the lipid nanoparticle or mRNA mechanism?” Clancy asked in the same Twitter thread. “Either way I am fascinated! Inflammation + tissue remodeling = extra bleedypants [sic]!”
https://twitter.com/KateClancy/status/1364671493507059713
It’s important to state that there is no data to suggest that any of the COVID-19 vaccines cause infertility or harm the reproductive system. In fact, it’s not yet known if the vaccine caused these changes. Of the millions of menstruating people who have already been vaccinated, at least 37 have officially reported painful, irregular, and/or heavier menstruation to the Vaccine Adverse Event Reporting System (VAERS).
But that didn’t stop the deluge of articles and online discussions about how changes in the menstruation patterns of Moderna-vaccinated individuals were proof that the vaccines weren’t completely safe. It prompted countless articles featuring prominent gynecologists labeling these effects as harmless — if they were even caused by the vaccine in the first place. Full disclosure: I wrote one of those articles myself.
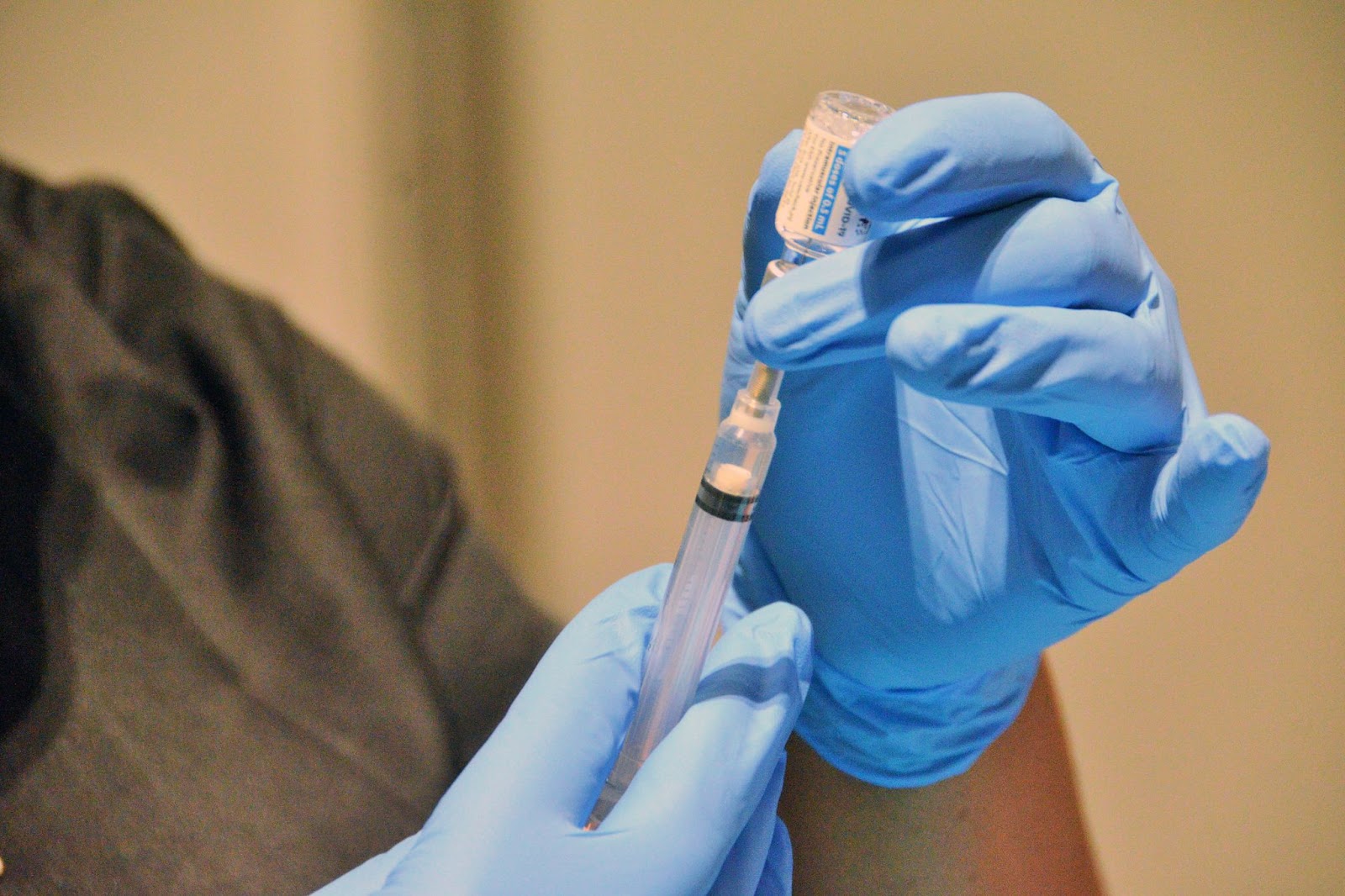
Now a larger conversation is taking place about the ways clinical trials address menstruation, and menstruating bodies. All it took were a few people to confide in one another — as has been done for centuries — to recognize a long-experienced gap in how science views the impact of drugs and vaccines on periods.
To better understand why these side effects weren’t disclosed to the public, one needs to explore the history of clinical trials, their relationship with menstruating participants, and the greater cultural understanding of what periods are.
A Brief History of Women and Clinical Trials
“It’s important to understand that clinical trials really have only been a thing since the 1940s,” Lara Freidenfelds said. Freidenfelds, who holds a doctorate in the history of science, has explored extensively the subjects of parenting, health, and reproduction as they are experienced in the US. Her first book, The Modern Period: Menstruation in Twentieth-Century America, won the Emily Toth Prize for Best Book in Women’s Studies.
It wasn’t until the 1970s that advocates started fighting for more humane clinical trials after instances of participant abuse came to light. In 1978, the Society for Clinical Trials was established to discuss and set trial standards when it came to design and analysis. A year earlier, the Food and Drug Administration (FDA) banned all women of “childbearing potential” from participating in clinical trials.
It was also in the early ‘70s when, according to historian Amy Bix, feminists started reflecting on the ways they were treated by their doctors and by the medical field at large.
“Among the issues that some women started to pay attention to were inequities in medicine, and in particular was a group of young women in Boston who started getting together to compare notes,” Bix, a historian in science, technology, and medicine at Iowa State University, said. “And they realized just how frustrated they were with the individual treatment by doctors where they would go and the doctor would dismiss their concerns as imaginary, but not explain things.”
The women relayed disturbing conversations that were had with their doctors, including instances where husbands were asked about their wives’ breasts during mammograms because, as Bix stated, women were reportedly “too emotional” about them. The conversations by this group of young women resulted in the book Our Bodies, Ourselves by the Boston Women’s Health Book Collective.
While feminists were beginning to discuss the treatment of women in medicine, there was still much to be done about their inclusion in clinical trials. The AIDS epidemic of the 1980s kicked off more modern clinical trials; those infected with HIV/AIDS were eager to participate in these trials as — at that time — it was their only chance of survival. Women were still not allowed in the earliest stages of vaccine or drug trials in an effort to protect them from becoming, as Freidenfelds put it, “human guinea pigs.” Only healthy men were accepted into these trials, allowing researchers to have a “cleaner” sample; that is, one without too many variables based on race or sex, in line with the scientific ideology of the time that marked men as the scientific standard while, according to both Freidenfelds and Bix, treating women as a departure from this.
“The problem is that because so much of the early research had been done on men, medical textbooks tended to hold up a standard of what was commonly known as the 70 kilogram man,” Bix explained. “So you’d open a medical textbook and it would say things like, ‘The effects of this medication have been calculated based on a 70 kilogram man.’ And the problem is we know now that medicine just doesn’t work that way. We know that there are important differences in the population; among other things, there are differences by sex.”
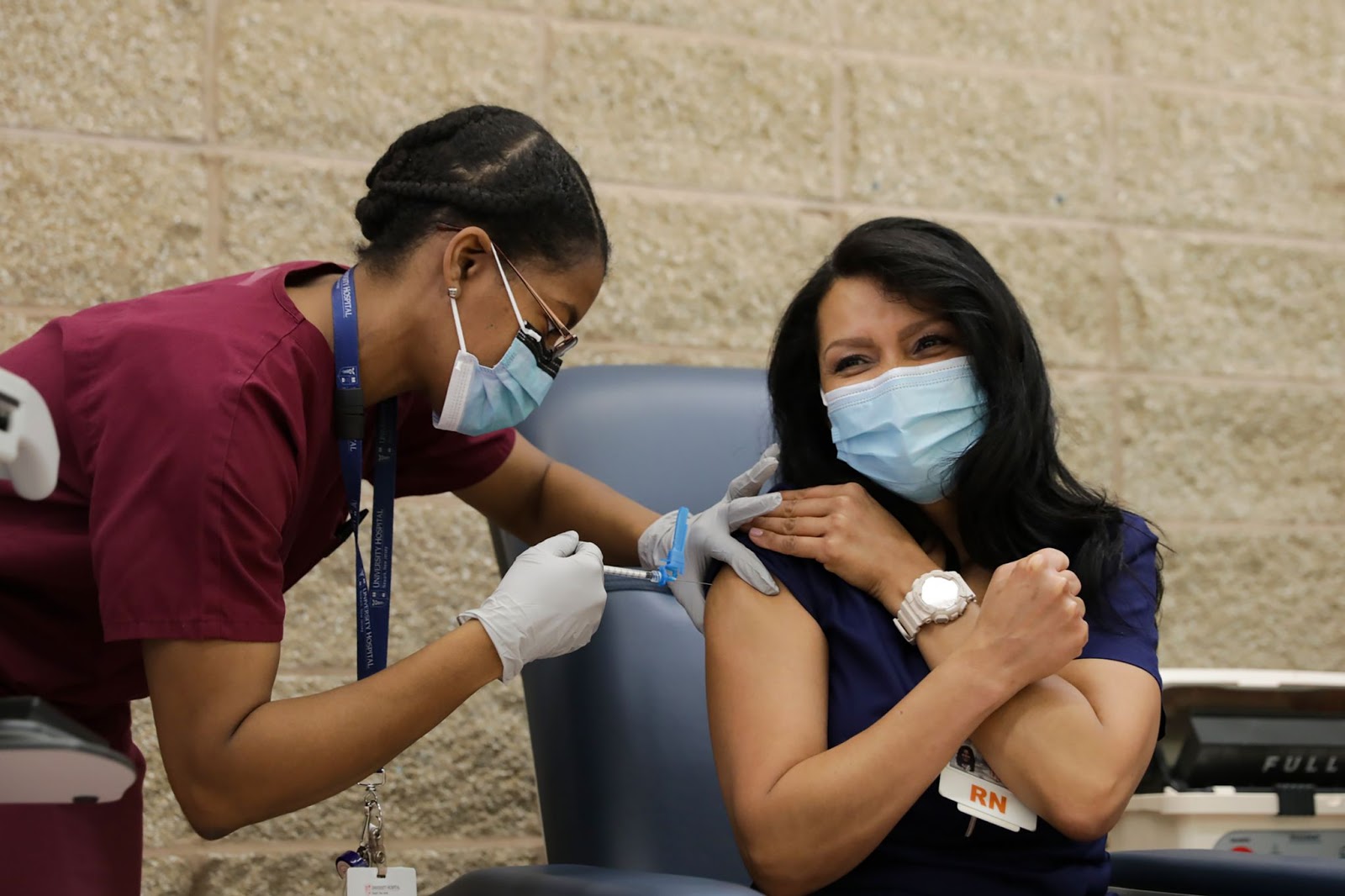
“We’ve treated women a little bit like a [separate] class of patients. … Somehow it’s been easy to ignore them or exclude them, and it’s particularly weird because it’s 50 percent of the population,” Freidenfelds said, commenting on how women were viewed in a similar way as those with critical health conditions.
“How do they become similar to someone who’s in chemotherapy?” Freidenfelds continued. “It’s because we have a very long term habit of seeing women as a minority somehow.”
That being said, few women wanted to participate in clinical trials. This was in part due to the widespread birth defects caused by the drug thalidomide in the late 1950s to early ‘60s. Initially seen as safe enough for pregnant women to take, the drug was marketed across 46 countries and sold as quickly as aspirin. Originally created as a sleep aid, thalidomide also alleviated morning sickness and was extensively prescribed to pregnant women without any study into side effects.
The situation ended badly, with over 10,000 children worldwide born with phocomelia — underdeveloped or missing limbs — as a result of their mothers’ thalidomide use. While the FDA didn’t approve the drug at the time, it is currently used to treat inflammation caused by leprosy and as chemotherapy for those with multiple myeloma.
The thalidomide scandal resulted in those who could become pregnant in the future — most menstruating people — being banned from clinical trials.
“Then there was really important political work done in the mid to late ‘80s, saying that the problem with not having women in clinical trials is you don’t understand how medications work in women’s bodies,” Freidenfelds explained. Based on these efforts, in 1994 the FDA finally rescinded its 1977 order, allowing women into every stage of a clinical trial.
People are looking for reasons to confirm their vaccine fears, and 37-plus women reporting period abnormalities after getting the Moderna shot did the trick.
Women’s Participation in Clinical Trials Today
Since the early days of regulated medicine in the US, clinical trials have become much more inclusive of the general population. Coronavirus vaccine producers, for example, made diversity and inclusion in clinical trials a pillar of their studies; 42 percent of Pfizer’s 46,331-person global trial were participants of color, with 50.9 percent identifying as female.
“It’s worth noting that there’s been even more attention in recent decades to the underrepresentation of minorities, and particularly minority women, in clinical trials,” Bix noted, explaining the need to continue diversifying clinical drug and vaccine trials. “When you’ve had white women under-studied, you’ve had black women or other minorities even more under-studied. So, in terms of fairness and in terms of ultimately scientific accuracy and medical benefit, that’s something that really needs to be addressed.”
For Freidenfelds and Bix, there are still many questions about the effect of vaccines on menstruation. Is there enough data from a given clinical trial to suggest that the participants’ periods were affected in general? How might birth control interact with the vaccine or drug being tested? Has the trial spanned several menstrual cycles to see if the effects are temporary or lasting?
The medical field is still trying to find an accurate method of determining what an “average menstrual cycle” is, leaving what some doctors refer to as the “fifth vital sign” up to interpretation.
“For reasons of trust … and because menstrual symptoms in other contexts are an indicator of life-or-death health conditions, it’s not a random thing I’m asking [doctors] for,” Freidenfelds explained. “It’s something that is a bodily indicator that in some circumstances is a crucial one. So when women want to feel that it’s being acknowledged, that’s a very legitimate perspective.”
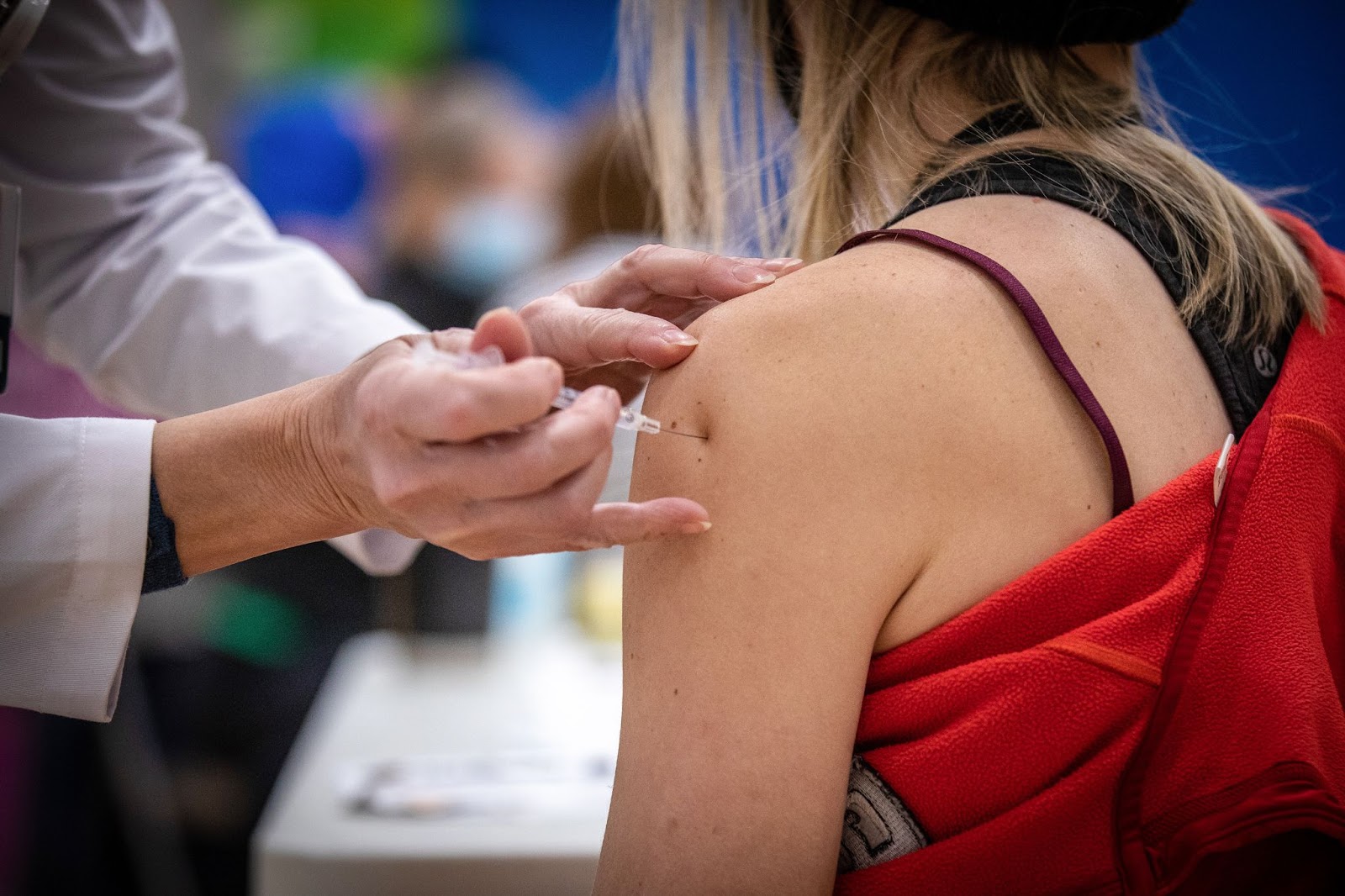
An Opportunity for Change
In a feat unknown to science of the past, three vaccines were developed, tested, and approved by the FDA in under a year. Moderna, Pfizer, and Johnson & Johnson provided the world with lifesaving vaccines and ensured that their clinical trials were as diverse as the global population. This was unheard of before 2020 and has set a new bar for vaccine creation in the future.
“What we’ve really seen was an unprecedented effort to develop a vaccine on a timeline that was far faster than anything before. It really was incredible,” Bix said. “It was amazing that we got the vaccines so quickly. And ultimately … they did a good job in the clinical trials as far as looking at the basic safety of the vaccine, trying to identify and detect what would have been extremely serious side effects. But in the process, they weren’t focused on necessarily asking all the questions they could have asked.”
Specifically, breaking down the trial data by gender then studying the vaccine effects, and the necessary dosages for each sex, that way.
“Clinical trials today do include women,” Dr. Sabra Klein, a professor of immunology and molecular microbiology at Johns Hopkins Bloomberg School of Public Health, said in an interview with the New York Times. “But in the trials for the new Covid vaccines, side effects were not sufficiently separated and analyzed by sex. And they did not test whether lower doses might be just as effective for women but cause fewer side effects.”
Even so, vaccine skepticism is at a high; with the anti-vaxxer movement, concerns over long-term effects of the vaccines, and disbelief in the virus’s existence, around one in four Americans are refusing to get vaccinated.
People are looking for reasons to confirm their vaccine fears, and 37-plus women reporting period abnormalities after getting the Moderna shot did the trick.
“In recent weeks, people who oppose Covid vaccinations have spread a claim that is not only false but defies the rules of biology: that being near someone who has received a vaccine can disrupt a woman’s menstrual cycle or cause a miscarriage,” reads a New York Times article titled “No, Other People’s Covid Vaccines Can’t Disrupt Your Menstrual Cycle.”
The article joins dozens of others confronting the claim that the Moderna vaccine, or someone else’s vaccine, could damage one’s reproductive system.
“One unfortunate side effect of women’s bodies having been under-studied for decades, is that amazingly enough, there’s still a lot we just plain don’t understand about just how complex women’s bodies, menstruation, and menopause are.”
Numerous experts have explained the possible reactions as completely normal and scientists have agreed that there is no proof definitively linking the COVID-19 vaccines to this reaction. However, misinformation and fear continue to spread.
“It’s absolutely important for women, and men, to pay attention to their bodies. On the other hand, it’s also important for everybody to really understand what’s going on here,” Bix said when addressing fears over the Moderna shot, and possibly other COVID-19 vaccines, causing damage to the recipient.
She noted that, as human beings, we have a bad sense of risk as well as a bad sense of correlation, or how variable A may be influenced by or linked to variable B.
“For that precise reason, it’s important that if you do suspect that the vaccine may, in some cases, affect women’s menstrual cycles, it’s important for people to be aware of that possibility so that, first of all, they don’t panic if something like that happens,” Bix said. “But then also, if they see problems continuing over subsequent months, to get it checked out by an OB-GYN, because that might turn out to be a symptom of something more permanent.”
In response to the flurry of attention brought to this issue, Clancy, with the help of colleague Dr. Katherine Lee, created an online survey to record the menstruation effects some are experiencing after the vaccine. Yet some question the validity of a survey like this.
“I don’t know even how you would set up a study that would look at that — everything would be anecdotal up to that point,” said Suzanne Junod, former historian for the FDA and current independent researcher, of the online survey. “If [the vaccine researchers] didn’t think to ask the question in the beginning, it’s kind of hard to go backwards.”
Not only this, but Junod said the resources and planning necessary to record each participant’s menstrual cycles throughout the duration of the study would make the process a challenging one to realize.
Junod noted that if researchers see a pattern of menstruation changes linked to the vaccine, whether it be during a trial or found retrospectively, this would become a factor in determining one’s candidacy and safety in clinical trials.
“When I went to get my shot, they listed off a bunch of things that might happen. So, if that was one of the things they wanted to list, [that] your menstrual cycle might change a little bit, that’s one thing,” Junod continued. “But saying ‘Don’t get it when you’re on your period,’ or ‘If you’ve got a birth control device, don’t use it or anything like that,’ that’s just a whole different can of worms. You’ve got to have a lot of evidence on that one.”
For Lee and Clancy, the goal of their study is to uncover whether there is in fact a link between the two, if the reactions are an immune response to the vaccine, or if the whole thing is just a coincidence.
“A lot of people had noticed something but hadn’t heard anything about [menstrual changes] being a side effect,” Lee told NBC’s Today. “So many things could impact people’s menstrual experiences. So, we just thought if this is a side effect of … this type of vaccine it would be good for people to be prepared.”
The survey joins a growing number of research efforts conducted by scientists, anthropologists, historians, and doctors in an effort to increase the attention paid to menstruation in clinical trials, and in general. It’s a project that will hopefully give insight into what Bix refers to as an “under-studied” aspect of scientific research.
“One unfortunate side effect of women’s bodies having been under-studied for decades is that, amazingly enough, there’s still a lot we just plain don’t understand about just how complex women’s bodies, menstruation, and menopause are,” Bix concluded.
For 30 years science has ignored the impacts of medical intervention on menstruation, resulting in a dearth of knowledge about periods. The Moderna vaccine, and the unnecessary fear it created, changed this; there’s no longer an option to avoid the effects of medications on menstruation. Instead, researchers, doctors, and academics can look into the void this event created and choose to make history.
Related front page panorama photo credit: Adapted by WhoWhatWhy from National Library of Medicine / Wikimedia.



