The harrowing trail of toxic nutrients in farm country water.
This story by Brett Walton originally appeared in Circle of Blue and is republished here as part of Covering Climate Now, a global journalism collaboration strengthening coverage of the climate story. This is the second of a two-part series. Read part one here.
AURORA, NE — Last October, a decade after their son Jacob died of a rare and aggressive form of lymphoma, Gary and Shari Peters reflected on an ordeal that produced unbounded pain, and unexpected clarity and purpose.
“There’s two ways to handle losing your child to cancer,” Gary said. “Get involved and do something or just disappear. There’s nothing in the middle.”
The Peterses took the first path. Gary, a construction project manager and volunteer assistant with the Aurora High School football team, turned his journals into a book-length chronicle of the family’s cancer year. He and Shari are active in the Pediatric Cancer Action Network, a grassroots advocacy and support group in Nebraska. Their work has revealed to them one of the darker sides of rural life in Nebraska. Six kids in town besides Jacob were diagnosed with cancer from 2005 to 2013.
An investigation by Circle of Blue uncovered compelling evidence for why — agrochemical contamination in Nebraska’s surface, ground, and drinking water. Pediatric cancer is more common in Nebraska than anywhere in the United States outside of the Northeast. And elevated numbers of pediatric cancer cases are associated with Nebraska watersheds that have high levels of nitrate (a fertilizer) or atrazine (a weed killer) in surface and groundwater, according to a University of Nebraska Medical Center research team.

Drinking water in rural Nebraska has become so prominent an issue that two state senators introduced bills this legislative session that target nitrate contamination. LB 1160 would use $10 million in federal coronavirus relief funds to assist rural communities in removing nitrate from their water. LB 925, meanwhile, would allocate $250,000 annually over five years to develop farmer-led educational programs on soil health and water quality.
Fresh attention to a persistent drinking water problem in farm country did not happen overnight. The University of Nebraska Medical Center research project traces its roots to Jacob’s cancer diagnosis a decade ago, a year of struggle that started innocently enough: with a bad game.
The evening of January 14, 2011, Jacob, then a 16-year-old sophomore at Aurora High School, entered a basketball game against Central City. In most contests for the Huskies, Jacob was a physical force. But that mid-winter day he faltered on the court. To Gary and Shari, the uncharacteristically sloppy performance and lack of effort were clear signs that their oldest son was ill.

Confirming their intuition, Jacob awoke the next morning congested with cold symptoms that developed into what Gary described as a “deep, heavy, hard, whole body cough.” A week of rest and antibiotics did not subdue the sickness. A different antibiotic didn’t either.
Two weeks later, Jacob was still having trouble breathing. At a January 31, 2011, appointment the doctor ordered blood tests and chest X-rays, to check for infection. The X-ray seemed off. A CT scan did, too. Medical staff shared worried glances. Biopsies the next day of Jacob’s lymph nodes and bone marrow resulted in the diagnosis the family had feared: lymphoma.
More specifically, it was T-cell lymphoblastic lymphoma, a rare and typically aggressive cancer that attacks the organs and tissues that rally the body’s defenses against disease. Within the week — and just three weeks after starting to feel ill — Jacob began chemotherapy in Omaha at the University of Nebraska Medical Center, a two-hour drive from the brick-paved streets of his 4,600-person hometown.
From the start he faced decisions few teenagers have to make. Did he want to participate in a clinical trial for an experimental cancer drug? Did he want to freeze his sperm, in case the cancer treatment robbed him of his ability to father children?
These were unexpected trials. All he wanted was to be in the weight room, preparing himself for his pivotal junior season of football, the year that college scouts would be assessing his potential and making scholarship offers.

In short time the rituals of Jacob’s life shifted. No more basketball practice and off-season football workouts. Instead, a buffet of medications, a tube inserted into his chest, and weekly trips to Omaha for treatment.
The University of Nebraska Medical Center is the only pediatric cancer care center in the state. The Peters family repeated the journey over and over and over. Gary and Shari estimated that they drove 12,000 miles during the course of Jacob’s treatment. They had to. Omaha was their closest option. Families in the western half of Nebraska, located unreasonably far from Omaha, turn in a different direction for care. They drive west, across the state line, to Denver, CO.
The burdens for families extend far beyond geography. Coulter cited data from Utah, which also has only one pediatric cancer center. A survey of 254 families that experienced a pediatric cancer found that one-third of adult caregivers quit work or changed jobs. Rural residents reported financial burdens due to the lengthy travel demands for hospital visits.
During Jacob’s treatment, both Gary and Shari lost their jobs. Shari’s layoff arrived out of the blue, a result of her employer closing the local office. Gary, who owned a construction company, fell behind on bills that stemmed from an apartment project three years prior that went over budget. He said that Jacob’s illness did not cause his company to collapse, but it might have accelerated the downfall. “I may have lost my will to fight two fronts during that time, but I believe now that it was inevitable.”
Many cancers, like tumors in the lungs due to smoking, have clear pathways for exposure. That is not the case for pediatric cancers like Jacob’s lymphoma. His doctors don’t know how he got it or what exactly he was exposed to. Don Coulter, the director of the University of Nebraska Medical Center’s Pediatric Cancer Research Group and one of the doctors on Jacob’s care team, said that pediatric cancer is a relatively rare occurrence compared to adult cancers. There is not a wealth of data to sift through. Jacob’s exposure could have taken place early in life or in the womb. It could have stemmed from epigenetic changes passed through the family. It could have resulted from the interplay between a basket of chemicals that are present in farm country.

Besides Jacob Peters, four of the Aurora kids died from their cancers. Tyler Larson was diagnosed in 2010 with neurofibroma sarcoma, which resulted in tumors on nerve endings. He was 19 when he died. Sydnee Owens, who contracted non-Hodgkin’s lymphoma in 2006, died six years later at age 14. Alyssa Sandmeier died at age 10 from leukemia. And Madalyn Spellman died at age 13 after being diagnosed with leukemia and bone cancer. Two kids survived and they or their parents did not want personal details published.
Even with the uncertainty around any individual’s disease, risk factors for nitrate contamination are not difficult to identify collectively. Septic systems, wastewater treatment plants, and lawns play a role. So does fossil fuel combustion. In countries without proper waste disposal, untreated sewage is a factor. And natural hazards like wildfire can elevate nitrate in streams. But the main source of nitrate is not the forest but the field. Where intensive, industrial-scale agriculture flourishes, nitrate is a menace.
A map of drinking water nitrate violations resembles a map of America’s high-value farm regions: California’s Central Valley and Washington’s Yakima Valley; the Corn Belt from eastern Nebraska through Iowa to Illinois; the Texas Panhandle; nearly all of Wisconsin dairy land; eastern Pennsylvania extending into the tri-state Delmarva region, where poultry operations dominate.
The towns at risk for nitrate in these areas share many characteristics. They are neighbors to the ag industry. They typically use groundwater. Groundwater systems account for nearly 95 percent of nitrate violations, according to the US Environmental Protection Agency. And they are small. Almost all nitrate violations occur in systems that serve fewer than 3,300 people. Especially vulnerable are the very small systems that have a population below 500. In other words, these at-risk towns look a lot like Creighton.
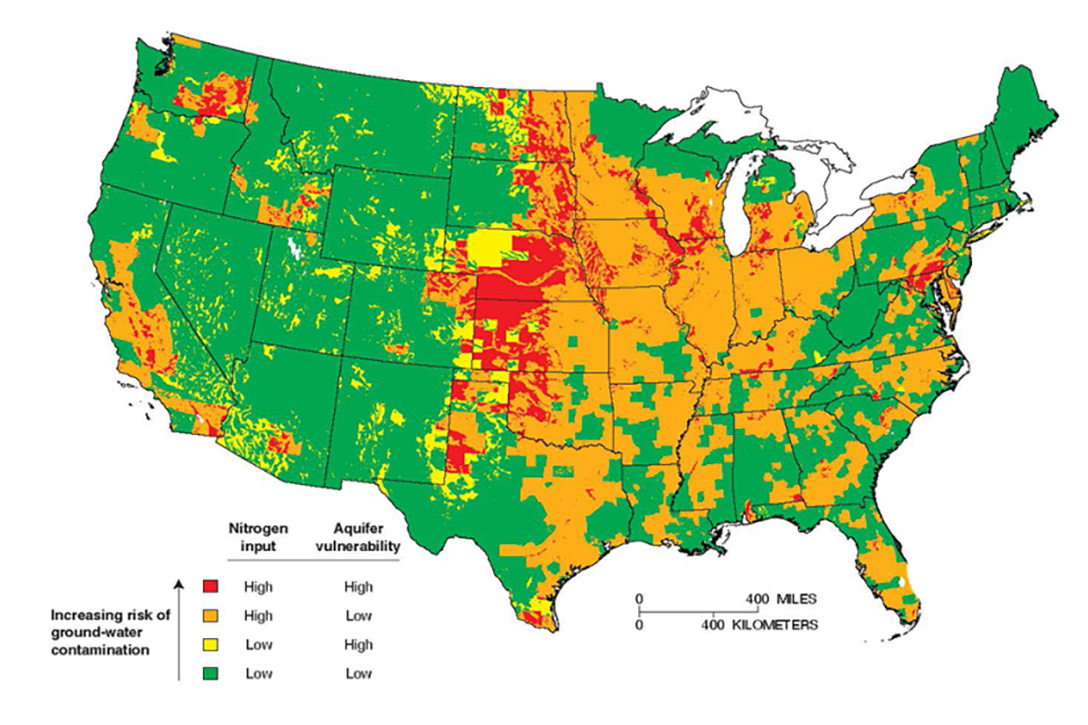
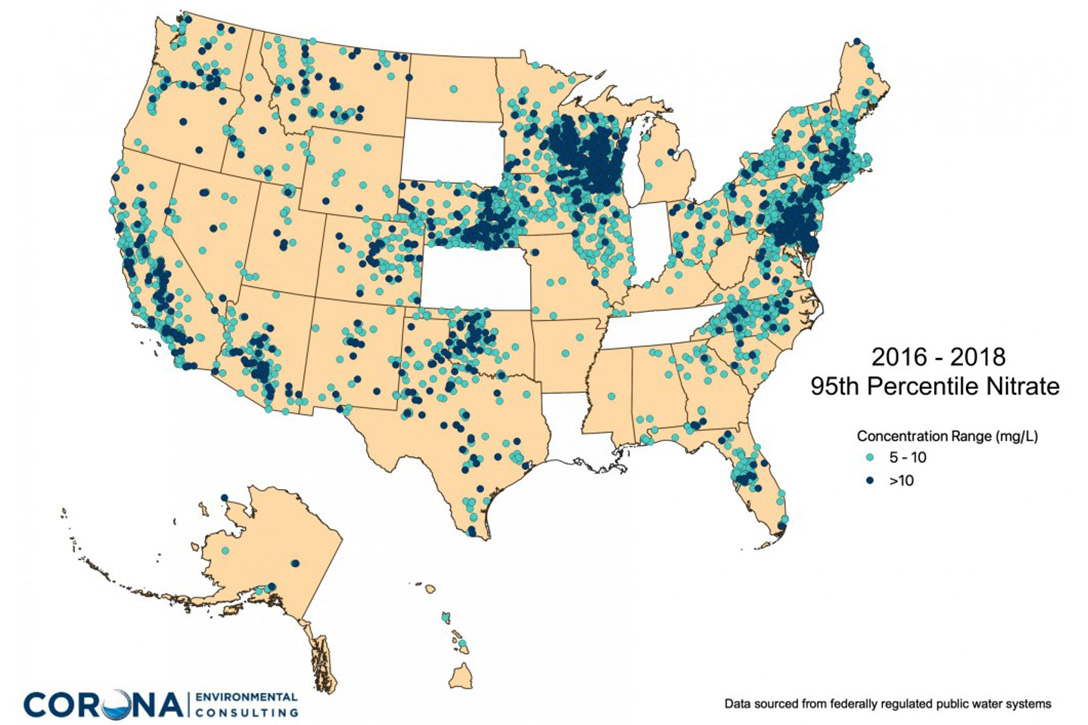
States shaded white did not provide or have data. The map shows a combination of nitrate and nitrate-nitrite data from state and federal sources. The map was produced by Corona Environmental Consulting based on a data-collection project funded by the Water Quality Research Foundation. Photo credit: Corona Environmental Consulting / Circle of Blue

First in Line
Creighton, like hundreds of small Nebraska communities, is surrounded by an expanse of corn and soybeans that ripples to the horizon, seemingly without end.
A small, tan building less than a mile east of Main Street has become a pilgrimage site of sorts. Not for religious seekers, but for town administrators and water professionals. The one-story structure at the intersection of state highways 59 and 13 houses the town’s nitrate removal facility.
Home to 1,147 people, Creighton was the first town in Nebraska to install reverse osmosis treatment for nitrate, opening the facility in 1991 at a cost of $1.3 million. It needs the facility in order to meet federal drinking water standards. Other communities do, too. Today, the Nebraska Department of Environment and Energy counts 49 public water systems in the state that have reverse osmosis systems for removing nitrate.

Kevin Sonnichsen, the town’s water commissioner, is responsible for running the facility. The annual operating cost, including electricity and cleaning the filters, is about $550,000. “It’s a money pit,” Sonnichsen told Circle of Blue.
Creighton’s present could be its neighbor’s future.
Plainview, another small farm town, is a 15-minute drive southeast of Creighton. The town has two wells, one of which began exceeding the federal nitrate standard in 2020.
Plainview has been down this road before. Town officials had to shutter two other wells because of high nitrate levels. When that happened they drilled new wells. Drilling yet another well will be a challenge. There are few nearby places where the groundwater isn’t already contaminated. If a new well doesn’t work out, then a reverse osmosis system like Creighton’s is a possibility.
Plainview is working with an engineer to determine the better option. Jeremy Tarr, the town administrator, is preparing to spend a lot. “We know it’s coming,” Tarr said. “We know it’s going to be a big number.”
Tarr worked in other small towns in Nebraska before taking the Plainview job in August 2020. None had nitrate problems, so Tarr is learning the ropes as he goes. He reckons a new well could cost $2 million. “That’s high for a small community,” Tarr said. If a new well is a high cost, a reverse osmosis system would be an astronomical outlay. Tarr will know more in the spring when the engineering reports are filed, but he’s anticipating maybe $8 million or more. “I’m not wanting to go down that road,” he said.
A helping hand for places like Plainview might be on the horizon. A bill introduced on January 19 in the Nebraska Legislature would provide $10 million in grants to rural communities for reverse osmosis treatment systems to remove nitrate. The money would come from the state’s allotment of federal coronavirus relief funds. LB 1160 was introduced by Sen. Anna Wishart, who represents Legislative District 27, an area that includes part of Lincoln and its southwest suburbs. The bill is scheduled to be heard by the Legislature’s Appropriations Committee on March 3.
Nitrate levels in Aurora fluctuate throughout the year, rising and ebbing with fertilizer cycles. At the maximum, nitrate in Aurora is just below the federal standard, though the town did exceed the 10 parts per million (ppm) threshold in the summer of 2017, registering 11.4 ppm.
For utilities that do not meet the current nitrate standard, the treatment options unfortunately are “complicated, onerous to operate, and expensive,” said Chad Seidel of Corona Environmental Consulting. And there is little enthusiasm among town water managers and utility operators for lowering the nitrate standard because of the cost and difficulty of meeting it at 10 parts per million.
The most common treatment option is ion exchange, a process in which contaminated water passes through a filter that swaps out nitrate for another type of ion, like chloride. Ion exchange works, Seidel said, but it has problems. The process introduces salts into the waste stream, which are detrimental for downstream waters. And these systems require savvy, well-trained operators. Tiny communities might not have access to such personnel.

A second option is reverse osmosis, the type of system that Creighton uses. Even that has drawbacks, Seidel said. It produces more corrosive water that could strip lead from pipes. Trained operators are also a requirement. Sonnichsen, Creighton’s water manager, wants to retire in a few years. Who, he wonders as the town’s population shrinks and ages, will replace him?
Communities nationwide are facing similar financial questions regarding nitrate. Ted Corrigan is the CEO and general manager of Des Moines Water Works, which is the drinking water utility for Iowa’s capital city. Des Moines is downstream from one of the most severe zones of agricultural water pollution in the country. Corrigan said that the utility’s $4 million nitrate removal facility, which was installed in 1992, costs $10,000 a day to operate.
It is turned on only when nitrate levels spike in the Raccoon River, one of its water sources. But the fact that the facility exists, Corrigan said, is an indictment of the state’s pollution-control measures. “It’s a cost that we shouldn’t have,” Corrigan said. “It’s a cost that’s inequitable, in my opinion.”
Jacob’s Road
Jacob’s treatment for T-cell lymphoblastic lymphoma started well enough. In those early months the family expected Jacob to join the 80 percent of pediatric lymphoma patients who survive the disease. “Everything is going according to plan,” Gary wrote in his journal on February 25, 2011. It was just before Jacob’s fourth chemotherapy session.
Weeks stretched into months. Despite the frequent trips to Omaha, Jacob’s schooling remained on track throughout the spring. He finished the semester with a 4.0 grade point average. Competitive sports, which, for Jacob, were the grand prize at the end of this dark tunnel, were a possibility again. At the end of May, his doctors allowed Jacob to begin summer football workouts. Gary joined him on that reintroduction to physical exertion.
“Bald, out of shape and of course wearing his mask, he still had spring in his step and an attitude that we have not seen since the diagnosis,” Gary noted in his journal on May 31.
Then the disease shifted course and the mood darkened. Jacob relapsed in June. He acquired a staph infection in July. A second relapse came in August. His doctors were anxious, The cancer had spread to Jacob’s blood and bone marrow. The best chance for survival, it seemed, was a stem cell transplant. It was scheduled for November, but Jacob kept relapsing, needing more chemotherapy. At that point, the disease broke him, his body no longer able to hold up.
Gary and Shari remain in touch with Don Coulter, Eleanor Rogan, and the rest of the University of Nebraska research team studying nitrates and childhood cancer. They plan to help collect water samples in Aurora for the next phase of research into the environmental factors of pediatric cancer. Anything they can do to find a cause or prevent other families from living their nightmare. “My long-term goal is to have it eliminated,” Gary said. “Just find out why. And fix that.”



