Caution: This Drug Trial May Be Harmful to Your Health
Will New Law and Industry-Friendly Trump FDA Endanger Patients?
A bipartisan health law that was recently passed ostensibly makes it easier for patients to get access to potentially helpful new drugs. But experts warn there could be serious side effects.
Who could oppose something called the 21st Century Cures Act? A bipartisan Congress embraced the legislation, passing the bill late last year. Sen. Lamar Alexander (R-TN) called it “a Christmas miracle.” It had the blessing of the Obama White House.
Not so fast, said some of the bill’s few Congressional critics. Sen. Elizabeth Warren (D-MA) warned that the bill had been “hijacked” by the pharmaceutical industry.
The bill authorizes Congress to invest billions of dollars in medical initiatives seeking a cure for cancer and other diseases, although it does not guarantee those funds will be appropriated. It also greatly streamlines the way new drugs get to the market, with the intent of bringing cutting-edge medical products to the public faster. But critics say the new law will fail to encourage innovation while jeopardizing the safety of patients.
Opponents are even more worried now that the power to implement the law will fall to a Food and Drug Administration (FDA) commissioner nominated by President Donald Trump. That nominee is likely to have strong industry ties.
What is at stake is the future of the FDA’s drug approval process, long considered the gold standard for the world. That could endanger all patients, particularly those taking antibiotics under FDA review. Indeed, in an op-ed last year, two Johns Hopkins physicians warned that the new law would create an FDA that would be “a shadow of its former self.”
To be allowed on the market in the US, drug companies have to demonstrate to the FDA that their drugs are safe and effective. The cornerstone of that proof always has been clinical trials. Patients who enroll in clinical trials must give their informed consent, after learning the potential risks and benefits of a new drug.
The new law will permit smaller clinical trials, and allow companies to include anecdotal evidence of benefits from individual physicians, patients, and caregivers to bolster their case for approval. It also eases the requirements for patient consent.
For example, just one provision, tucked deep into the 996-page bill, will make it easier for drug companies to be excused from informing patients about the harmful effects of a new drug if “the proposed clinical testing poses no more than minimal risk to such human beings.”
Writing in the New England Journal of Medicine, Harvard School of Medicine professors Jeffrey Avorn and Aaron Kesselheim termed informed consent a “sacrosanct” practice in drug trials, dispensed with only when it is “impossible to obtain or contrary to the patient’s best interests.” To no longer require informed consent when trials don’t pose much risk, they stated, is a “major departure” from patient protections, particularly when it’s “not clear who gets to determine whether a given trial of a new drug poses ‘minimal risk’.”
John Powers, a physician and professor of clinical medicine at George Washington University School of Medicine, told WhoWhatWhy that many other aspects of the new law are equally problematic. He points to new provisions for drug trials of antibiotics and says these changes in law could encourage trials that raise serious ethical and scientific questions.
Powers is an infectious-disease specialist who spent seven years at the FDA, where, as a lead medical officer for the agency, he was involved in its efforts to address antibiotic resistance and oversee the development of new antibiotics. He has written and co-authored 60 papers for medical journals, and testified before Congress three times.
Powers understands why Congress would want to develop more antibiotics, and agrees there is a problem. The Centers for Disease Control and Prevention (CDC) estimates that each year two million people in the US develop infections resistant to existing antibiotics, causing 23,000 deaths. But he contends that the new law will not achieve the goal Congress intended.
To a layman, the way the 21st Century Cures Act addresses drug resistance looks prudent. The new law encourages the development of more antibiotics by speeding up and relaxing the FDA approval process.

Specifically, the law encourages a less rigorous type of clinical trial and more expedited review for new antibiotics. In exchange for these less stringent standards, the FDA will require drug companies to carefully label their products, stating that they should be reserved for patients with “limited options” — meaning that they are essentially last resort drugs — to be used by patients with infections that can’t be treated with any other antibiotic. The new law requires the Government Accountability Office (GAO) to evaluate this approach and its impact and report back to Congress by 2021.
But there is more to the law. It also makes clear that the FDA cannot prevent drug companies from selling their products to patients who do not have a drug-resistant infection and could do just as well, if not better, on an older, cheaper antibiotic. And doctors have no restrictions on what they prescribe to patients, as long as a medical product is approved by the FDA.
The FDA and other supporters such as the Pew Charitable Trusts support this approach. Allan Coukell, Pew’s senior director for health programs, wrote in a 2016 blog that “there is an urgent need for action to spur the innovation of antibiotics to treat the most serious and life-threatening super-bugs.” Indeed, it is the specter of some global epidemic triggered by bacteria resistant to existing antibiotics that persuaded Congress and the FDA to go down this path.
Powers disagrees. The new law “really defies logic,” he says. The reason? The new drugs will not be tested on the patients who actually have infections that are resistant to all existing antibiotics. Instead, patients who have infections that already respond well to existing drugs will be the guinea pigs, in the hope that future patients may benefit.
There are two problems with this approach, Powers says. First, you’re putting patients who could do well on older, more proven drugs at risk, often without adequate informed consent. And, second, even if the newer drug works well enough in these patients, you still have not demonstrated that the new drug will work on the patients for whom it was intended, who likely are older and sicker.
In the past, when it came to drugs for infectious diseases, clinical trials generally compared new drugs to placebos or other non-antibiotic therapies. There were few antibiotics on the market in the 1930s to 1940s, Powers says. These trials were called “superiority trials” because they tried to determine whether a new drug worked better than either an older drug or other accepted treatments.
Antibiotics proved to be “remarkably effective” in saving the lives of patients, “remarkably better than available therapies at the time,” he says. “But over the past 30 years something changed.”
The clinical trial that drug companies like to use, and that the new law will encourage for antibiotic development, is different. It’s called a “noninferiority” trial. One might reasonably assume that “noninferior” means that the new drug under review is not inferior to the old drug. But that’s not what the term means in this context. In fact, it means the opposite. It means that the new drug under review is just as, if not more, likely to be less effective than the established drug.
“Most clinical trials start out with the question, ‘Does it work better?’ Because that’s what patients and clinicians want to know,” Powers says. “Noninferiority trials ask, ‘Does it work a little worse?’”
Why would anybody want to test a new drug they already think probably works less well than an older drug? Because the new drug might be just a little less effective, but have fewer side effects, or be easier to take. These trials aim to measure how much less effective a new drug is, and also identify other benefits it may offer that may still make it worth approving.
It is not difficult to understand why drug companies pushed Congress to encourage these types of clinical trials, Powers says. When drug companies have to prove their product is better than the existing product, their clinical trials have a success rate of about 50 percent. When their products are judged on how much less effective they are, the trials have a 96 percent success rate. That is because these trials assess whether a new drug falls below a measure set by investigators ahead of time. For example, many noninferiority trials aim to demonstrate that a new drug is up to ten percent less effective than an available effective drug. Of course, as more and more drugs are approved through noninferiority trials, the likelihood increases of getting drugs approved that are less and less effective.
Nevertheless, Powers agrees that noninferiority trials have their place in medicine, under three conditions: when drugs are treating ailments that are not life-threatening; when the new drug offers some other benefit to patients, like fewer side effects; and when patients are able to give informed consent before enrolling in the trial, knowing they are making tradeoffs between less effectiveness and some other benefit.
But what several research studies have found, he says, is that many clinical trials of antibiotics fail to meet these conditions. Patients are not asked in the informed consent process whether they are willing to be treated with a drug that may not work as well but may have fewer side effects or be easier to take. Some patients may be willing to accept the tradeoffs, Powers says. But others may not. They all deserve to make that choice, a cornerstone of ethical trials for nearly 50 years, he says.
Worse, patients with life-threatening illnesses also are in clinical trials where they may be receiving a less effective drug that may actually kill them, he says. That danger, he notes, is not hypothetical. The FDA has warned of increased risk of death for several new antibiotics.
Powers and his colleagues recently completed their review of the information that patients receive when they agree to participate in clinical trials comparing two drugs. Their study, which has not yet been published, reviewed consent forms for 72 clinical trials of 17 new antibiotics, with three-quarters of the trials focused on serious diseases. None of the consent forms explained to patients that the purpose of the study was to see whether the new drug might be less effective than a drug currently on the market. Indeed, four consent forms implied the new drug was safer and more effective.
This may not be a crisis when a patient has a mild infection, and takes a drug that is three percent less effective, particularly if the new drug has fewer side effects, Powers says.
But that’s not the case when patients have life-threatening infections like pneumonia, Powers says. “Pneumonia can kill you. Why would you accept any less effective drug? If you have a life-threatening illness, you don’t want to trade away any effectiveness.”
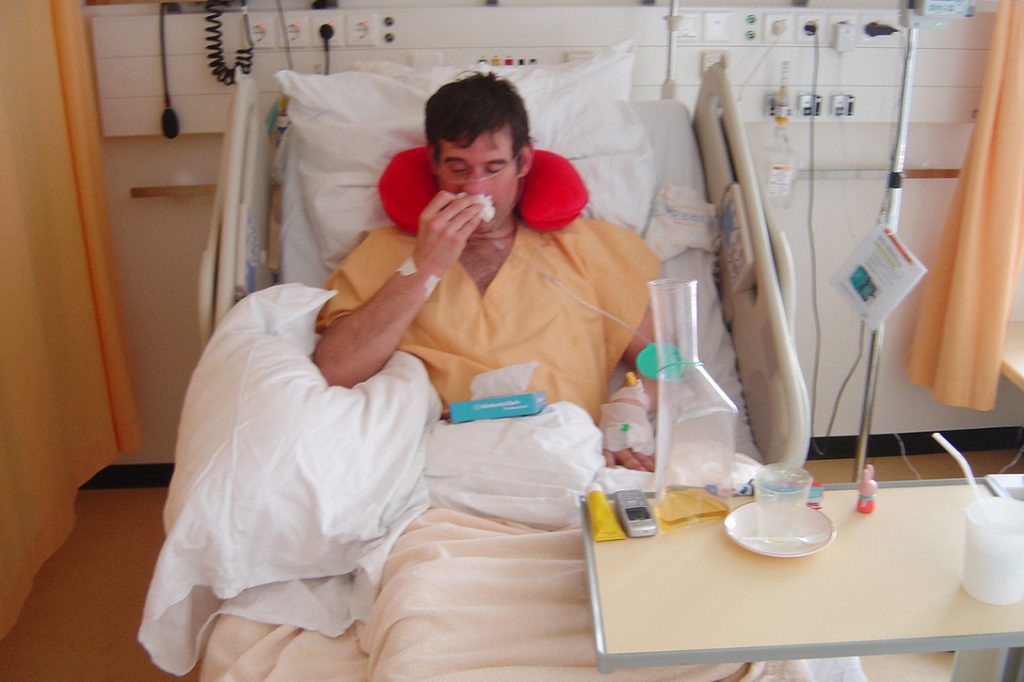
Powers insists that drug companies ought to be testing their new antibiotics on the patients who really need them, those who are out of options because they have an infection that is resistant to existing drugs. Patients who have effective options should not be the “stand-ins” for patients without options, he says.
Not everybody agrees with Powers’s assessments. Coukell, Pew’s health advocate, responded to WhoWhatWhy by email. He wrote that Pew does not take a position on clinical trial design, and leaves that to the FDA to oversee and monitor. But he contended that these trials compare new drugs that may either be marginally better or less effective than existing drugs.“You’d love it, if the new drug were superior, but if it is just as good, you also want it to be available.” He stated that it would “never be ethical to enroll a patient in a trial if you had reason to believe” one drug was “better than the other.” And he noted that noninferiority trials are used for many other medical conditions and types of drugs, not just antibiotics.
Coukell also observed that it would be very difficult for drug companies to do clinical trials on patients whose infections are resistant to current antibiotics.” One big difference between cancer and bacterial infections is time,” Coukell wrote. “Someone with an infection needs an antibiotic immediately, which makes it much harder to find people and get them into trials.” However, he agreed that “it would be good if we were better at enrolling patients in clinical trials.”
Coukell predicted that this type of trial — comparing an existing antibiotic to a new drug — is likely to be the way antibiotics for life-threatening infections are going to come to market. “The real challenge is how to respond to that small but growing number of patients who have an infection that can’t adequately be treated with existing antibiotics. If I have one of those infections, I may be willing to take a drug where there is less certainty, than I would if I had lots of options.”
But Powers insists that is the point. Patients with infections known to be resistant to all antibiotics may be willing to take the risk, but patients with other options have no reason to accept any increased risk, he says. The only way to address the problem is to do a straight-up superiority trial where you give the new antibiotic to patients with no other options and see whether the drug works, compared to the best current standard of care.
That likely would also mean that the drug would be given to older, sicker patients and would better reflect how the drug would actually work on the patients who need it the most. He adds that this approach also could stimulate the development of better diagnostic tools to test and use these new drugs on the people most likely to benefit, making it easier to quickly identify and enroll these patients in clinical trials.
That is how cancer drugs are usually tested, Powers says. The new drug is given to patients who are not responding to current drugs to see if it helps. It is not given to patients whose cancers are responsive to existing treatments.
The new law also permits new antibiotics to come to market through trials that are smaller. The goal is to get new, effective antibiotics into the pipeline faster. But trials for antibiotics already are faster and require fewer patients than trials for other types of drugs.
And Powers says small trials have been largely unsuccessful. For one thing, an individual trial might show promising results in a small group but not identify the drug’s problems. Powers points to the drug Tygacil, approved by the FDA to treat complicated infections.
It was only in 2010, after a meta-analysis of 13 clinical trials, that the FDA found a significantly higher risk of death among patients taking Tygacil, compared to other antibiotics used to treat similar conditions. It required a “black-box” label on the medication, warning of the increased risk of death.
Another published study examined eight new antibiotics treating life-threatening diseases approved by the FDA between 2010 and 2015. The study concluded that while these new drugs often were ten times more expensive than existing antibiotics, it was unclear whether they were any better.
The clinical trials evaluating the drugs did not report whether the drugs actually cured patients or helped them recover from their symptoms or live longer. Instead, the trials relied on subjective physician assessments of patients’ health, and lab results.
Often, Powers says, insurance companies won’t pay for far more expensive antibiotics if they have not proven to be more effective than the older, cheaper drugs.
Indeed, an evaluation of antibiotics approved by the FDA between 1980 and 2009 found that more than four in ten were withdrawn from the market over time, either because of safety problems or due to poor sales.
“The public health cost of this is enormous,” Powers says. “Over 39,000 patients enrolled in studies to allow drugs to be approved that are usually more expensive, that are not shown to be better, and can be worse than what we have already, in the hopes that one of these drugs will remain useful in the future, while the evidence shows most of them are not. This is an inefficient use of resources, as well as putting thousands of patients who have effective options at risk.”
The full impact of the new law remains unknown. Even though few new antibiotics have sold well in the recent past, will more lenient standards coax more investment from drug companies into antibiotic research and development? Will the new law embolden drug companies to more aggressively promote new antibiotics to patients who do not need them? Will a new Trump administration lean on Medicare and other health insurers to pay for costly new antibiotics, even if they are less effective?
Powers says he understands the need for new antibiotics and the problem of antibiotic resistance. But he regrets that Congress and the FDA are not focused on what makes more sense for patients and practitioners — developing better ways to find patients with superbugs that are resistant to all existing drugs, and testing new drugs on them, “so we can find out what really works in the people with the greatest need.”
Doing anything else, he says, “is not science and medical practice based on evidence. It ignores doctors’ duty to ‘first do no harm’ and replaces it with wishful thinking.”
Related front page panorama photo credit: Adapted by WhoWhatWhy from pills (Images Money / Flickr – CC BY 2.0).